Melasma Causes and Treatment- A Complete Guide
What is Melasma
Melasma is a very common skin pigmentary condition. Melasma is associated with brown, or unusually darker colour than your skin natural colour patches on the skin. It is a form of skin hyperpigmentation typically triggered by sun and UV exposure, hormonal factors such as consumption of oral contraception, or internal hormonal changes that happens during pregnancy.
Those with darker skin, like Asians, have higher probability of melasma. This is because their skin naturally consists of more active pigment-producing cells, also known as melanocytes. Melasma also occurs more frequently in women than men due to higher level of oestrogen, progesterone and melanocortin hormone especially during pregnancy. It is also believed that genetic predisposition plays an important role in the cause of developing melasma.
Signs and Symptoms
You can identify melasma as darkened patches on your skin, usually on sun exposed areas- the forehead, cheeks, nose or even upper lip. Regardless of its size, they are generally symmetrical blotchy patches that are noticeably different from the rest of your skin.
Causes of Melasma
Melasma can be triggered by sun exposure, genetics and hormonal changes.
Sunlight is considered the principal factor that triggers melasma. This happens when ultraviolet rays affect the cells that control pigment/colour (melanocytes) leading to excessive melanin production.
It also affects individuals with a genetic inclination to this condition, for example Asians, Middle Eastern and Hispanic backgrounds and those with genetic history of melasma condition. Melasma, however, is rare in individuals with extreme Fitzpatrick skin types, such as skin type I (Western) and VI (African).
Fluctuating hormones tend to increase the risk of developing melasma. Those who rely on oral contraceptive use and other hormonal therapies are particularly at risk of melasma attacks. It appears that estrogen and progesterone sensitivity are associated with the condition as melasma tend to develop during pregnancy, after starting birth control or when undergoing other hormonal treatments.
Types of Melasma
As of now, there are four types of pigmentation patterns diagnosed in melasma:
1. Epidermal
2. Dermal
3. Mixed (epidermal and dermal)
4. An unnamed type found in dark-complexioned individuals
The epidermal type is the most superficial with an increase in the skin pigment (melanin) in the top layer of skin (epidermis) while in dermal melasma, there is increased skin pigments in the deeper layer of the skin (the dermis). Mixed refers to combination of epidermal and dermal melasma.
In the fourth type, excess melanocytes are present in the skin of specific dark-skinned individuals.
How is Melasma diagnosed?
Melasma is diagnosed through clinical examination, meaning there is no specific tests required to confirm the skin condition. A trained doctor will be able to identify melasma just by visual inspection though the doctor may check your skin under a device called a Wood’s light to differentiate the types of melasma to ensure his diagnosis.
If your doctor is concerned that the discoloration may be caused by serious skin conditions, a skin biopsy may be performed but this is rare.
Treatment options for Melasma
If you are diagnosed to have melasma, there are treatment options can greatly reduce facial hyperpigmentation. Your doctor may also suggest combination treatment for best and soonest outcome.
Preventive treatments – Sunscreens
One of the main methods to treat and prevent melasma is with proper application of sun protection. As sun exposure is the primary trigger for many, diligent application of sunscreen during day time, regardless of weather is encouraged. The strength of sunscreens matters as well, and the general recommendation is between 30 – 50 SPF with reapplication every two hours. If the sun is particularly relentless, or if you are in midst of activities under the sun such as hiking, swimming or cycling, you should reapply sunscreen more frequently.
Medications and Creams and how they work
As melasma mostly affects the face, these patches can cause distress and embarrassment.
Conventional treatments for melasma include sunscreens and creams. These medications can be over-the-counter or for prescription-strength medications, to be prescribed by doctors or dermatologists. A popular and proven ingredient that help treat melasma is hydroquinone with 2-4% concentration.
For severe melasma cases, blended creams with triple-combination of active ingredients of hydroquinone, tretinoin, and steroid are recommended for better potency.
The below explains how each ingredient combat melasma:
1. Hydroquinone:
Hydroquinone helps to lighten the patches. It is available in cream, lotion, gel or liquid form. Those sold over the counter are generally less potent and may not be as effective as the ones prescribed by your doctor/dermatologist.
2. Tretinoin:
This substance enhances and expedites the effects of hydroquinone, thus increasing its efficacy.
3. Corticosteroid:
While tretinoin speeds up skin cell turnover, corticosteroid helps reduce inflammation.
Many skin doctors promote prescription products that contain all three ingredients above as they have been proven to help combat melasma. Melasma patients have reported improvement in their condition after a few months of usage.
Microdermabrasion
Microdermabrasion is a non-invasive procedure that exfoliates the epidermis (superficial layer of dry, dead skin cells) and because this procedure helps increase cell turnover, it helps to get rid of cells already affected by discoloration and thus reduces the appearance of melasma.
However benefits are best seen after a series of microdermabrasion treatments so it does not offer instantaneous results.
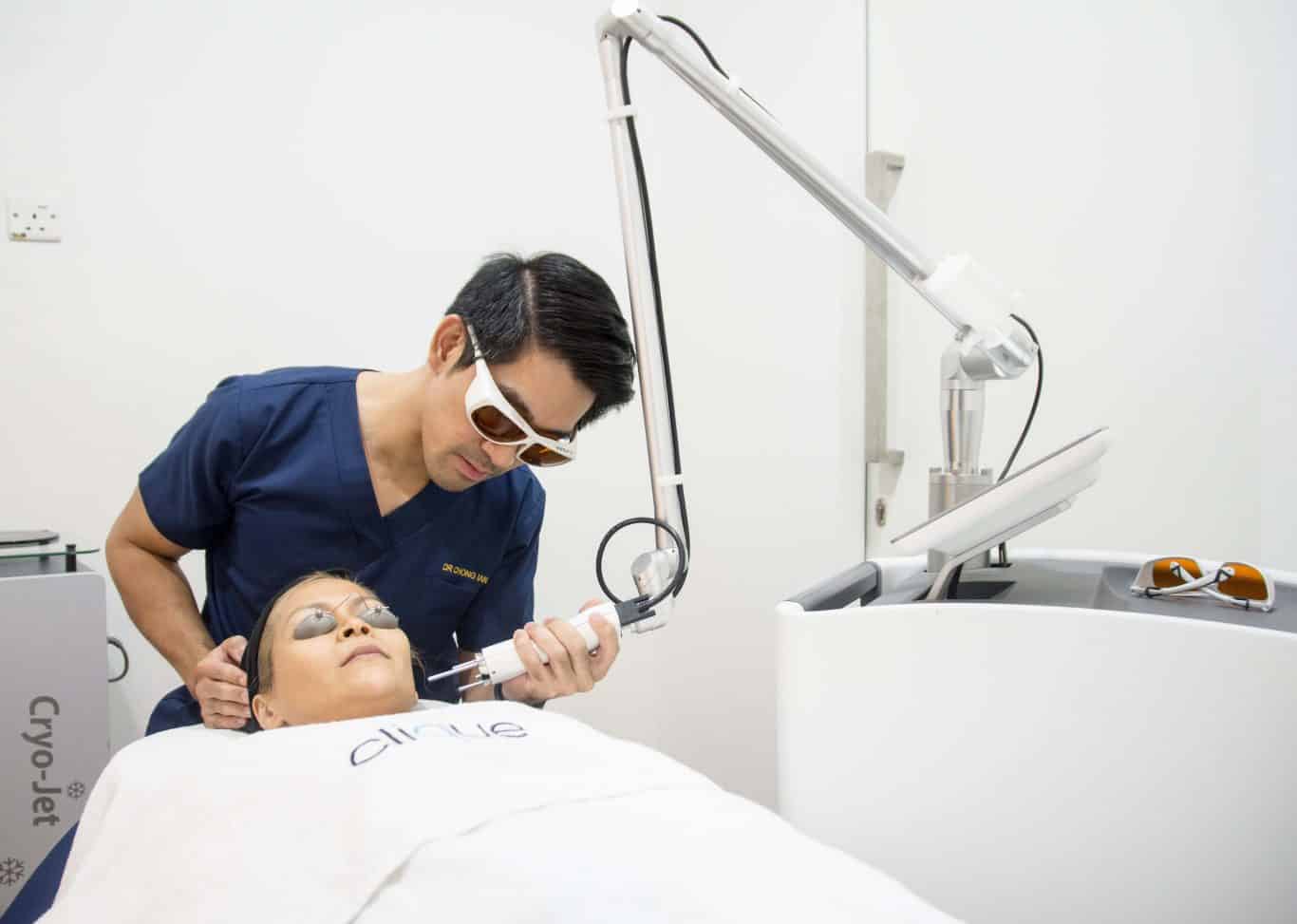
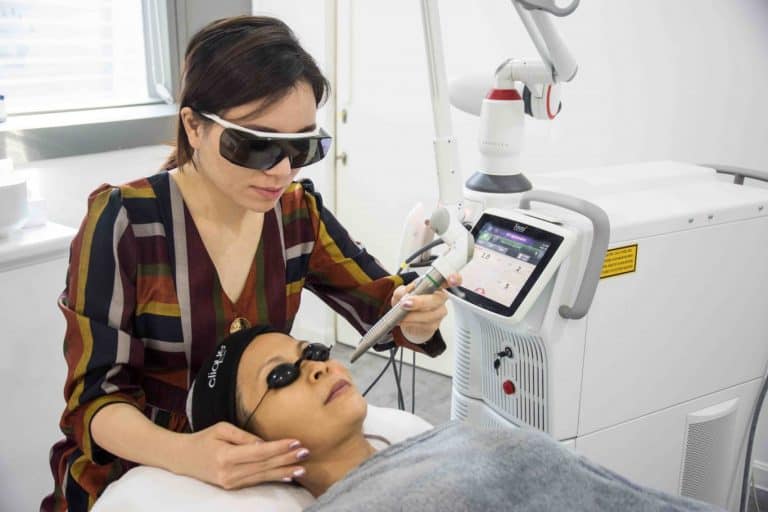
Laser treatment
In recent years specific lasers have been proven to be effective in treating melasma. Though several sessions are required for gradual improvement, laser’s efficacy for melasma has been well-documented and favourable for its success rate with low recurrence. One of the most effective melasma-busting laser treatments are Q-Switched and Pico Laser.
Chemical peel
Peeling agents as skin resurfacing treatments are an attractive alternative in the treatment of melasma.
How it works is by removal of unwanted melanin by causing a controlled destruction to the skin surface (epidermal), leading to exfoliation and removal of superficial skin which is followed by the regeneration of new epidermal and dermal tissues. As such, new skin takes over the old, and gradually the melasma spots fade away.
Chemical peels have proved to be effective for melasma, either as a sole treatment or with the aid of topical applications.
Light Therapy
In addition to chemical peels, microdermabrasion and topical creams, intense pulsed light, low frequency lasers are good alternatives for effective melasma removal and particularly beneficial for patients who wishes for an accelerated pace of improvement.
How light therapy and lasers work are by selective destruction of pigments with specific wavelengths of radiation while sparing the surrounding tissues.
Laser and light therapy for the treatment of melasma are recommended for patients with refractory melasma and had failed to experience significant improvements with topical treatment or after a series of chemical peels. Topical therapy requires consistent application for a minimum of three months or more before apparent results. Patients who suffers from more severe melasma or keen for rapid improvements may consider laser and light therapy.
Risks and Side effects
The current treatment options for melasma are chemical peels, microdermabrasion, lasers and topical creams, all of which involves peeling of the skin surface to induce skin regrowth or application of creams that are skin-bleaching agents with primary function to lighten areas of darkened skin.
The risks and side effects of such treatments are avoidable with a well-defined procedure and post-op care. One of the most common side affects is post-inflammatory hyperpigmentation (PIH) following a peel or an ablative laser.
Outlook and Prognosis
Melasma can to be a chronic skin disorder with unpredictable breakouts and recurrent attacks.
In some cases, it can disappear with no treatment, especially if the case is triggered by pregnancy or birth control pills. In many instances, however, melasma can persist for a long time. However technology breakthroughs has increased the prognosis for melasma. Research has shown that the successful disappearance of melasma is based on establishing the right treatment combination for each individual skin type.
Choosing a reliable provider
Melasma is a skin condition so it is imperative to seek the professional advice of certified aesthetic doctors for appropriate treatments.
Certifications
Dermatology is the branch of medicine dealing with skin disorders. It is a specialty with both medical and surgical aspects. As melasma is a skin disorder, recommended medical practitioners are reputable and certified aesthetic doctors and dermatologists; physicians who specialise in skin disorders.
Cost of treatment
As treatments for melasma varies, the cost of treatment is similarly different. Topical creams would certainly cost lesser than lasers and chemical peels, but the efficacy and speed of result would not match those of lasers. Depending on the severity of the melasma and skin condition, a series of treatments or multi-modality procedures may be necessary.
Often, what works for an individual may not work for another, and therefore, various discourses may be necessary. As of now, it is challenging to spot a specific procedure that is most effective for melasma.
Conclusion/Final thoughts
While melasma can be treated, the right procedure largely depends on the severity of your melasma. As the skin type and lifestyle of every individual are unique, no one treatment plan is guaranteed to work. If you are diagnosed with melasma, be sure to discuss with your dermatologist to identify the best treatments that may help.
No procedure can guarantee that melasma won’t reoccur, and in some cases of melasma the patches can’t completely vanish. Lifestyle changes are required to maintain the results of treatment, or you may have to maintain consistent treatment to reduce the risk of the melasma returning.