What Is The Main Cause Of Melasma?
Melasma is a common skin pigmentary condition, especially in Asia. It can be triggered by sun exposure, genetics, hormonal changes and history of skin irritation.
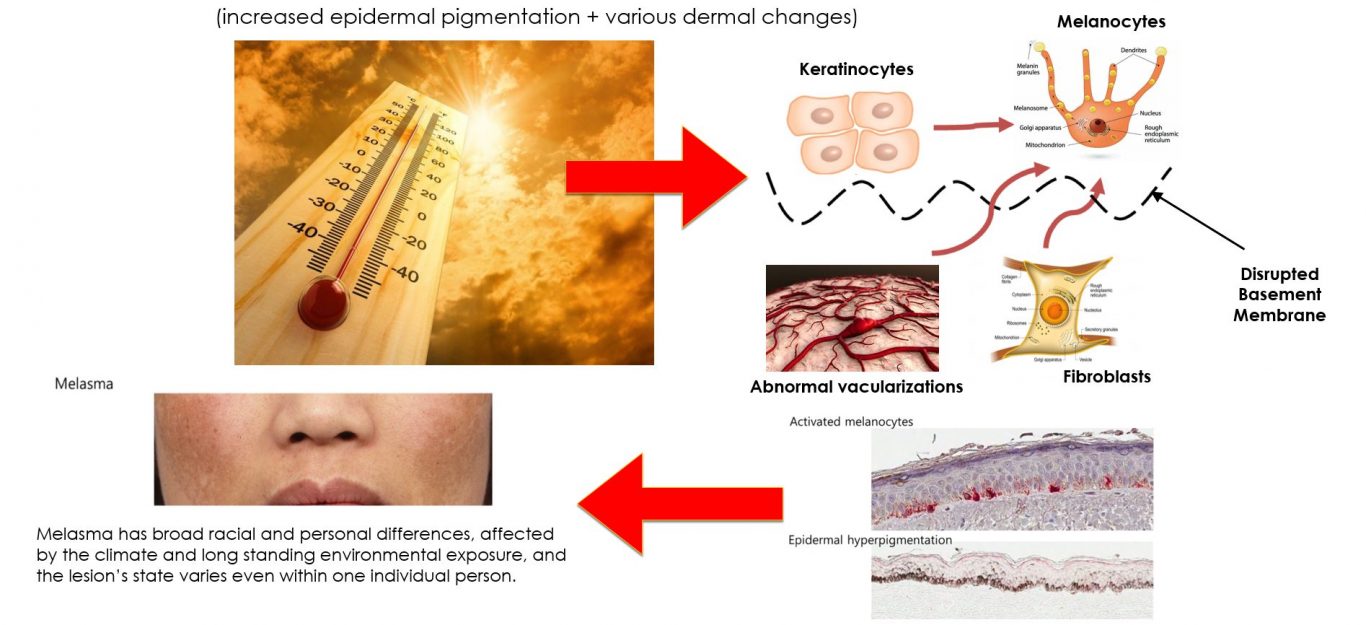
Ultraviolet (UV) radiation is considered the principal factor that triggers melasma. This happens when ultraviolet rays stimulate the cells that control pigment/colour (melanocytes) leading to excessive melanin production which causes brown or grey patches to appear on the face area of the skin.
Melasma is also very much linked to our skin health, especially the basement membrane of our skin. The basement membrane is the structure in between the superficial skin (epidermis) and the deeper skin (dermis). Most people will find that their melasma is very stubborn to treatments because the disruption of the basement membrane that makes it resistant to creams, or lasers alone.
About Melasma
The bridge of the nose, forehead, cheeks and upper lips are common areas for melasma. Women of the South East Asia descent, or risiding in South East Asia (Malaysia, Singapore, Thailand, Philippines, Laos, Cambodia, Myanmar, Vietnam) countries are more prone to get melasma due to their skin structures1 as well as chronic exposure to UV radiations from very young age. Also, besides genetic, hormones also play a part, as pregnant women are more likely to develop melasma.
Men can also develop melasma, but it is not very common. According to the American Academy of Dermatology, only 10% of all melasma cases involved men.
What is pigment (melanin)?
The pigment melanin is responsible to define the colour of a person’s eyes, hair, and skin. The exposure from the sun, genetics, hormonal changes, inflammation and age can affect the production of melanin. Hyper-pigmentation is the result of the over-production of melanin which contributes to the appearance of dark spots and uneven skin tones. In contrary, underproduction of melanin (hypo-pigmentation) causes the skin to look fairer than the skin arounds it.
Types of Melasma
There are three types of melasma; epidermal, dermal and mixed.
1. Epidermal melasma affects the top layer of the skin causing a well-defined border of brown patches due to the pigmentation.
2. Dermal melasma affects the deeper dermis level where the patches are in blue-grey patches.
3. Mixed melasma (a combination of epidermal and dermal) shows brown-grey patches. This type of melasma is harder to treat than the other two.
Identifying Symptoms of Melasma
The obvious symptom that can be observed with the naked eye is the development of discoloured patches on the skin. Experienced doctors can tell the types of melasma and the treatment options for it, but for most cases in South East Asia, we see very mixed types of melasma.
Causes of Melasma
The causes of melasma is complex and involved many structural changes2. It may be due to the malfunction of melanocytes (colour-making cells) which then triggers the over-production of pigments for normal skin. People with darker skin complexion are prone to develop melasma due to the number of melanocytes that they have in comparison with lighter-skin people. Other potential triggers for melasma are the changes in hormone (caused by pregnancy, hormone replacement therapy (HRT) or birth control pills), chronic sun exposure when younger and using skincare products that irritates the skin. Lastly, genetics play a factor as well.
Changes in hormone
The changes in hormone that may be responsible for melasma are pregnancy hormones, hormone replacement therapy (HRT) or birth control pills. During pregnancy, endogenous hormones stimulate melanocytes to produce more melanin pigments. This subsequently causes the number of melanin pigments to be imbalanced and contributes to the cause of melasma. Women that undergo hormone replacement therapy and those taking birth control pills share similar hormonal changes as those that occur during pregnancy.
Chronic sun exposure
UV exposure is a major factor in the development of melasma. Most people do not recognise that the melasma is due to long years of sun exposure that continues to damage the basement membrane in the skin. After years of damage, the skin finally gave in and become more prone to having hyperpigmentations.
More often than not, darker skin types with more melanocytes, which if triggered, increases the production of melanin in their body and thus expose them to the risk of having melasma. Avoiding the sun and applying broad-spectrum high-factor sun protection are two simple but effective habits in avoiding the stimulation of pigment production.
Skin care product
Certain skincare products are not suitable for those with sensitive skin as irritation might occur. Therefore, careful choice of skincare product is important.
Genetic
Genetics play an important role in the development of melasma. An individual is also more susceptible to melasma if there is a positive family history of the condition.
Treatment options
If you are diagnosed to have melasma, there are treatment options can greatly reduce facial hyperpigmentation. Your doctor may also suggest treatment combinations for the best and soonest outcome.
Restoration
Restoration of the skin health is the most important step in managing melasma. Therefore repairing the basement membrane, and restoring the basement membrane function using devices such as Sylfirm or Sylfirm X is very crucial. Without these steps, many people with melasma will have rebound cases or worsening of the melasma after years of using lasers or creams.
Removal
This treatment is via laser therapy, intense pulse light or chemical peel and has been proven to help treat melasma. Potential side effects may include inflammation, irritation and a burning sensation.
Laser therapies (Picogenesis, PicoSure, Q-Switched, Aerolase, Glacier Rx)
Laser treatments are more precise than chemical peels. In laser therapies, high-energy lights are used to target the affected area as it removes hyper-pigmented skins cells at the surface or deeper level, depending on condition severity. In the new era, good quality picosecond laser with very mild energy is important to help clearing the melasma without causes long term side effects. Also the use of cooling technology such as with Glacier Rx will be helpful in the long term treatments of melasma.
Chemical peels
Glycolic acid (AHA) is used frequently by aesthetic doctors and dermatologists for chemical peeling. It induces the top layer of the skin to peel off and increase the skin cells turnover. As the skin sheds, new, unblemished skin will be revealed. This is only effective in mild and not complicated melasma. It should not be used in darker skin types, especially in tropical countries.
To regulate skin colouration, here are the few ingredients typically present in topical medical or skincare products to treat melasma.
Conclusion/ Final Thoughts
While melasma can be treated, the right procedure largely depends on the severity of your melasma. As the skin type and lifestyle of every individual are unique, no one treatment plan is guaranteed to work. If you are diagnosed with melasma, be sure to discuss with your aesthetic doctors or dermatologists to identify the best treatments that may help.
No procedure can guarantee that melasma won’t reoccur, and in some cases of melasma the patches can’t completely vanish. Lifestyle changes are required to maintain the results of treatment, or you may have to maintain consistent treatment to reduce the risk of the melasma returning.
References
1. Goldie K, Kerscher M, Fabi SG, Hirano C, Landau M, Lim TS, Woolery-Lloyd H, Mariwalla K, Park JY, Yutskovskaya Y. Skin Quality – A Holistic 360° View: Consensus Results. Clin Cosmet Investig Dermatol. 2021;14:643-654
https://doi.org/10.2147/CCID.S309374
2. A review of combined treatments for melasma involving energy-based devices and proposed pathogenesis-oriented combinations. Joseph N. Mehrabi, Efrat Bar-Ilan MD, Shehadeh Wasim MD, Amir Koren MD, Lior Zusmanovitch MD, Fares Salameh MD, Gila Isman Nelkenbaum MD, Tamir Horovitz MD, Eyal Zur RPh, Ting Song Lim MD, Jacob Mashiah MD, Ofir Artzi MD. J Cosmet Dermatol. https://doi.org/10.1111/jocd.14110




